A Complete Guide to Prescription Management Software Development
Table Of Content
Published Date :
21 Apr 2026
Key Takeaways
- Digital prescription systems are becoming essential for modern healthcare operations
- Automation reduces errors and improves efficiency across workflows
- Compliance with regional regulations is critical for long-term success
- Custom-built solutions offer better scalability and alignment with business needs
- Investing in the right system improves both operational performance and patient experience
In an era where medication errors contribute to nearly 9,000 deaths annually in the United States alone, and where regulatory bodies are tightening controls around controlled substances, healthcare providers and pharmacies are rapidly moving toward intelligent, automated prescription management systems.
Healthcare systems across North America are under visible strain. In Canada alone, over 60% of physicians report administrative overload impacting patient care rel="nofollow", while in the U.S., medication errors contribute to thousands of preventable cases annually.
This is where prescription management software development begins to shift from a “nice-to-have” to a strategic necessity. Clinics, pharmacies, and telehealth providers are no longer just digitizing records, they’re rethinking how prescriptions move through their entire ecosystem.
This guide breaks down how modern prescription systems are built, what businesses should actually look for, and why getting this right can directly impact operational efficiency and patient trust.
What is Prescription Management Software
Prescription management software is a system that handles the creation, tracking, and processing of prescriptions in a digital environment. But in practice, it does far more than that.
It connects physicians, pharmacies, and patients into a single workflow where prescriptions move securely and instantly, without the friction of manual intervention.
Think of a busy clinic handling 200 patients a day. Without a digital system, prescriptions get handwritten, passed around, sometimes misread. With a structured system in place, everything becomes traceable, standardized, and faster.
How Medical PMS Fits into Modern Healthcare Workflows
Today’s healthcare environment is interconnected. A prescription doesn’t sit in isolation. It links with patient records, insurance systems, pharmacy inventory, and even follow-up care.
A well-built medical prescription management software ensures:
- Real-time prescription sharing between providers and pharmacies
- Automatic validation against patient history
- Reduced back-and-forth communication delays
- Seamless integration with clinical systems
Key Users Across Prescription Management Software Ecosystem
This type of system isn’t limited to one segment. It supports:
- Pharmacies managing daily dispensing operations
- Hospitals handling high patient volumes
- Clinics streamlining consultations
- Telehealth platforms enabling remote prescribing
And here’s the reality. As healthcare becomes more digital, businesses that don’t adopt such systems often find themselves stuck with inefficiencies that scale quickly.
Are Your Prescription Workflows Slowing Down Care Delivery?
Identify inefficiencies, reduce errors, and streamline operations with a system designed around real healthcare workflows and scalability needs.
Why Healthcare Businesses Need Prescription Management Software
Healthcare leaders today are dealing with a difficult balance. Rising patient expectations on one side, operational pressure on the other. Somewhere in between sits prescription handling, often overlooked, yet critical.
Growing Patient Load and System Pressure
Walk into any urban clinic or hospital and you’ll see it. More patients, less time. Physicians are expected to process consultations faster, without compromising accuracy.
Manual prescription workflows simply don’t hold up under this pressure. They slow down consultations and increase the risk of errors.
Reducing Errors and Improving Safety
Medication errors are not rare edge cases. They happen more often than most executives assume. A misread dosage or incorrect drug interaction can lead to serious consequences.
A structured pharmacy management system introduces checks that humans can’t consistently maintain under pressure, such as:
- Automated drug interaction alerts
- Allergy checks based on patient history
- Standardized prescription formats
Meeting Regulatory Expectations
Compliance isn’t optional, especially in regions like Canada and the USA. Regulations such as PIPEDA and HIPAA demand strict handling of patient data.
A digital system ensures:
- Secure data transmission
- Controlled access based on roles
- Audit trails for every action
Businesses that delay compliance upgrades often face higher costs later, both financially and reputationally.
Enhancing Patient Experience
Patients today expect convenience. They don’t want delays, unclear prescriptions, or repeated visits due to errors.
A streamlined system improves:
- Faster prescription processing
- Reduced waiting times at pharmacies
- Better coordination between providers
As healthcare systems become more patient-centric, businesses are increasingly aligning prescription workflows with broader healthcare app development strategies.
This allows patients to access prescriptions, track medications, and receive updates directly through mobile applications, creating a more connected and accessible care experience.
When patients notice smoother service, trust builds naturally. And in healthcare, that trust translates into long-term retention.
Key Features of Prescription Management Software
A well-designed AI-powered pharmacy management software focuses on reducing friction, improving accuracy, and saving time where it matters most.
Core Functional Capabilities
- E-prescription creation and digital transmission: Prescriptions are generated digitally and sent instantly to pharmacies, eliminating delays and handwriting errors.
- Patient and medication history management: Every prescription ties back to a detailed patient profile, ensuring continuity of care.
- Drug interaction and allergy alerts: The system flags potential risks before the prescription is finalized, adding an extra safety layer.
- Integration with EHR and EMR systems: Seamless connectivity ensures that prescriptions align with clinical records without duplication.
Operational And Financial Features
- Billing, insurance, and claims integration: Insurance validation happens alongside prescription processing, reducing administrative workload.
- Pharmacy inventory management: Real-time stock visibility helps avoid last-minute shortages and improves dispensing efficiency.
- Reporting, analytics, and audit trails: Decision-makers gain insights into prescription trends, operational bottlenecks, and compliance status.
Here’s the kicker. When these features work together, they don’t just improve efficiency. They quietly remove daily frustrations that staff often accept as “part of the job.”
Struggling With Prescription Errors And Compliance Risks?
Explore how automation, validation checks, and secure systems can minimize risk while ensuring compliance with evolving healthcare regulations.
Types of Prescription Management Software
Not every healthcare business needs the same kind of system. The choice depends on scale, complexity, and long-term goals.
Standalone Pharmacy Systems
Pharmacies use these systems which they designed to handle dispensing and inventory management and prescription tracking tasks. The system operates effectively in standalone environments, but its capabilities become restricted when used by extensive healthcare organizations.
Integrated Hospital and Clinic Solutions
Hospitals and multi-specialty clinics need systems which connect prescription processing with their complete operational workflows that include diagnostics and billing and patient record management.
Integration serves as the essential element of this process. The initial performance of an unconnected system functions properly, yet its operational weaknesses increase as the organization expands.
Cloud-Based Vs On-Premise Systems
| Factor | Cloud-Based Systems | On-Premise Systems |
| Accessibility | Accessible from anywhere | Limited to local infrastructure |
| Maintenance | Managed by provider | Managed internally |
| Scalability | Easy to scale | Requires hardware upgrades |
| Cost Structure | Subscription-based | Higher upfront cost |
Across Canada and the USA, cloud adoption is growing rapidly due to flexibility and lower maintenance overhead.
Custom-Built Vs Off-The-Shelf Solutions
Off-the-shelf tools are quicker to deploy but often lack flexibility. Custom solutions, on the other hand, align closely with specific workflows.
And here’s where many businesses hesitate. Custom development seems complex. But in reality, it often saves time in the long run by eliminating workarounds.
Prescription Management Software Development Process
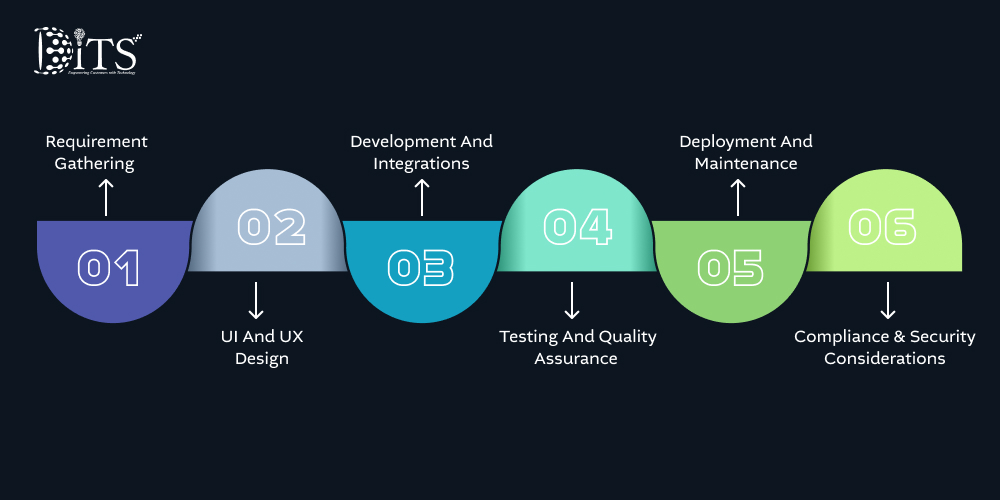
Building a reliable software requires a clear understanding of how healthcare workflows actually play out in real environments, where time is limited, decisions are critical, and even small inefficiencies can create large operational challenges.
Requirement Gathering
Everything starts with clarity. What workflows need improvement? Where are the bottlenecks?
For example, a mid-sized clinic might struggle with prescription turnaround time, while a hospital may face integration challenges across departments.
UI And UX Design
Doctors and pharmacists don’t have time to “figure out” software. Interfaces must be intuitive, fast, and aligned with real workflows.
A poorly designed interface can slow down operations more than a manual system.
Development And Integrations
This phase focuses on building core functionalities and connecting with systems like EHRs, insurance platforms, and pharmacy databases.
At DITS, this is where we bring in AI in healthcare capabilities, not as a buzzword but as a practical layer that enhances validation, automation, and decision-making across the system.
Testing And Quality Assurance
Healthcare software cannot afford errors. Every feature goes through rigorous testing to ensure accuracy, security, and compliance.
And guess what? Even small glitches can disrupt workflows significantly, which is why testing isn’t rushed.
Deployment And Maintenance
Once deployed, the system must adapt to real-world usage. Regular updates, performance monitoring, and user feedback loops keep the system relevant.
A system that isn’t maintained quickly becomes outdated. And in healthcare, outdated systems create risks.
Looking To Reduce Costs And Improve Efficiency Fast?
Unlock operational savings, reduce manual workload, and accelerate prescription processing with a scalable, future-ready digital solution.
Compliance and Security Considerations
Healthcare data isn’t just sensitive, it’s heavily regulated. And for businesses operating across Canada, the USA, or both, compliance isn’t a one-time task. It’s an ongoing responsibility.
Regional Regulatory Requirements
- In Canada, regulations like PIPEDA and provincial health data laws govern how patient information is collected, stored, and shared
- In the USA, HIPAA sets strict standards for protecting patient data and ensuring privacy
If your system doesn’t align with these frameworks, it’s not just a technical gap. It becomes a business risk.
Data Protection Measures
A secure medical prescription management software must include:
- End-to-end data encryption during transmission and storage
- Role-based access control to restrict sensitive information
- Audit logs that track every action within the system
These aren’t optional features. They form the foundation of trust.
Cross-Border Data Handling
Here’s where things get complex. Many healthcare providers operate across regions or use cloud systems hosted in different countries.
That means your software must:
- Comply with multiple regulatory standards simultaneously
- Ensure secure data transfer across borders
- Maintain transparency in how data is accessed and stored
Miss this, and compliance gaps start showing up in audits.
Cost of Prescription Management Software Development
Cost discussions often get reduced to a single number. In reality, it’s a layered investment shaped by scope, compliance, and long-term business goals.
For healthcare businesses in Canada and the USA, the cost of building a reliable system typically falls within a predictable range, but the variation depends on how complex and integrated the solution needs to be.
Key Cost Factors
- Feature complexity and customisation level
- Integration with existing systems like EHRs and insurance platforms
- Compliance and security requirements
- Scalability and performance expectations
A basic system may take a few months to build, while a fully integrated enterprise solution can take significantly longer.
Estimated Cost Breakdown
| Solution Type | Estimated Cost Range (USD) | Typical Timeline |
| Basic system (limited features, standalone) | $40,000 – $65,000 | 2 to 4 months |
| Mid-level solution (integrations, compliance-ready) | $65,000 – $100,000 | 4 to 7 months |
| Advanced system (enterprise-grade, fully integrated) | $110,000 – $500,000+ | 7 to 12+ months |
Hidden Costs Businesses Often Overlook
Here’s where many decision-makers get caught off guard:
- Integration costs with legacy systems
- Data migration from existing platforms
- Staff training and onboarding
Ongoing maintenance and updates (typically 15% to 20% of initial development cost annually)
Ignore these, and budgets can stretch unexpectedly. Plan for them, and the investment becomes far more predictable.
ROI Perspective
The real value of prescription management software development shows up after deployment.
Reduced administrative workload, fewer prescription errors, and faster processing times are the primary advantages that helps organizations saves time and cost. In many mid-sized healthcare setups, operational efficiency improvements can recover initial investment within 12 to 24 months.
And beyond numbers, there’s something harder to quantify but equally important. Fewer errors, fast and quality patient care and the most important, better patient trust.
Ready To Modernize Your Prescription Management System?
Transform outdated processes into a connected, efficient digital ecosystem that improves speed, accuracy, and overall patient experience.
Benefits of Prescription Management Software for Healthcare Businesses
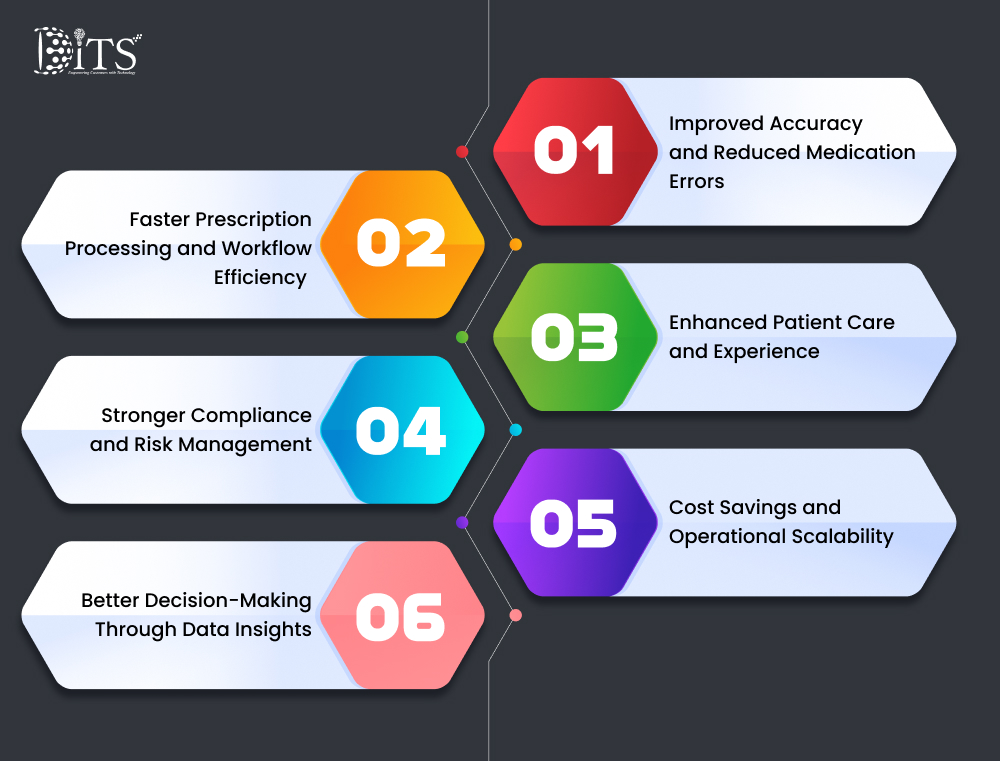
When healthcare leaders evaluate new systems, the conversation often starts with efficiency. But in reality, the benefits go much deeper. A well-implemented pharmacy management system doesn’t just streamline operations; it reshapes how care is delivered, measured, and experienced.
Improved Accuracy and Reduced Medication Errors
In high-pressure environments, even experienced professionals can make mistakes. A handwritten prescription, a missed allergy note, or a dosage oversight can lead to serious consequences.
Digital systems introduce built-in safeguards that work silently in the background. They validate prescriptions against patient history, flag potential drug interactions, and standardize formats across the board.
Over time, this reduces error rates significantly. And more importantly, it builds clinical confidence across teams.
Faster Prescription Processing and Workflow Efficiency
Speed matters, especially when patient volumes are rising. In a typical clinic, delays in prescription handling can create a ripple effect, longer queues, overworked staff, and frustrated patients.
A structured pharmacy management software eliminates unnecessary steps by:
- Automating prescription generation and transmission
- Reducing manual data entry
- Enabling real-time communication between providers and pharmacies
Here’s what that looks like in practice. A physician completes a consultation, generates a prescription within seconds, and the pharmacy receives it instantly. No paperwork. No follow-ups. Just a seamless flow.
Enhanced Patient Care and Experience
Patients rarely see the backend processes. But they feel the impact.
Shorter waiting times, fewer errors, and clearer communication create a smoother experience. And in healthcare, even small improvements matter.
For example, when prescriptions are accurately transmitted and ready before the patient arrives at the pharmacy, it removes a common frustration point. That small change? It leaves a lasting impression.
Stronger Compliance and Risk Management
Compliance isn’t just about meeting regulations. It’s about avoiding costly disruptions.
A digital system ensures that every prescription, every update, and every access point is recorded. Audit trails become easy to generate. Data access is controlled. Security protocols are consistently enforced.
This reduces the risk of non-compliance penalties and simplifies audits, which, in regulated markets like Canada and the USA, can otherwise become complex and time-consuming.
Cost Savings and Operational Scalability
At first glance, investing in software may seem like an added expense. But over time, inefficiencies cost far more.
Manual workflows require more staff hours, increase error-related costs, and slow down operations. A digital system addresses all three.
- Reduced administrative workload
- Lower error-related expenses
- Improved staff productivity
And as your organization grows, the system scales with you. No need to rebuild processes from scratch.
Better Decision-Making Through Data Insights
Modern systems don’t just process prescriptions. They generate data that can guide business decisions.
You can track:
- Prescription trends across locations
- High-demand medications
- Operational bottlenecks
This kind of visibility allows leadership teams to move from reactive decisions to proactive planning.
And that shift? It’s where real competitive advantage begins.
Future Trends in Prescription Management Software Development
The healthcare landscape is changing rapidly, and prescription systems are evolving alongside it. What was once a basic record-keeping tool is now becoming an intelligent, connected platform.
AI-Driven Prescription Validation and Automation
Artificial intelligence is moving from experimentation to real-world application.
In prescription workflows, AI is being used to:
- Analyze patient history for risk patterns
- Suggest alternative medications based on outcomes
- Automate routine validation processes
This doesn’t replace clinical judgment. It enhances it.
At DITS, we integrate AI not only into the software itself but also into development, testing, and optimization processes, ensuring that systems remain adaptive and continuously improving.
Expansion of Telehealth and Remote Prescribing
The rise of virtual care has changed how prescriptions are issued and managed.
With telemedicine in healthcare, patients can consult doctors remotely and receive prescriptions without visiting a physical clinic.
This shift requires systems that support:
- Secure remote prescription generation
- Direct digital transmission to pharmacies
- Integration with virtual consultation platforms
And here’s the catch. As telehealth adoption grows, businesses without integrated prescription systems will struggle to keep up.
Mobile-First Healthcare Solutions
Healthcare professionals are no longer tied to desktops. Mobile accessibility is becoming a standard expectation.
Modern systems are being designed to work seamlessly across devices, allowing providers to:
- Generate prescriptions on mobile devices
- Access patient records on the go
- Respond to updates in real time
This flexibility improves responsiveness and ensures continuity of care, especially in fast-paced environments.
Real-Time Analytics and Decision Support
Data is becoming central to healthcare strategy. But raw data alone isn’t enough. It needs to be actionable.
Advanced systems now offer real-time dashboards that provide insights into:
- Prescription volumes and trends
- Medication usage patterns
- Operational efficiency metrics
This enables leadership teams to make informed decisions quickly, rather than relying on outdated reports.
Integration With Broader Healthcare Ecosystems
Prescription systems are no longer standalone tools. They are becoming part of a larger digital ecosystem that includes:
- Electronic health records
- Insurance platforms
- Remote monitoring tools
As solutions like remote patient monitoring gain traction, prescription systems will play a key role in continuous patient care, ensuring that medication management aligns with real-time health data.
Prescription systems are evolving from basic tools into intelligent platforms that support both clinical and business decision-making.
Why Choose DITS For Prescription Management Software Development
Choosing the right development partner isn’t just about technical skills. It’s about finding a team that understands healthcare workflows, compliance requirements, and long-term scalability.
As a custom software development company, DITS focuses on building solutions that align with real-world healthcare operations across Canada, the USA, and global markets.
What Sets DITS Apart
- Deep expertise in healthcare software development, tailored for complex healthcare environments
- Strong understanding of regional compliance requirements across North America
- Custom-built solutions designed around your workflows, not generic templates
- End-to-end support, from planning and development to deployment and scaling
We also integrate AI across our development lifecycle, from coding and quality assurance to customization, ensuring that every system is efficient, adaptive, and future-ready.
The result? Software that doesn’t just function but evolves with your business.
Want A System Built Around Your Healthcare Operations?
Move beyond generic tools and implement a custom solution tailored to your workflows, integrations, and long-term business goals.
Conclusion
Prescription workflows may seem like a small part of healthcare operations. But in reality, they sit at the centre of patient care, compliance, and efficiency.
As healthcare systems become more complex, relying on outdated or manual processes is no longer sustainable.
Investing in the right digital solution is not just about technology. It’s about building a system that supports your teams, protects your patients, and scales with your growth.
For businesses willing to make that shift, the long-term impact is hard to ignore.
FAQs
What is prescription management software development?
It refers to the process of designing and building digital systems that help healthcare providers create, manage, and track prescriptions efficiently and securely.
Is prescription management software compliant with Canadian and US regulations?
Yes, when developed correctly, it aligns with regulations such as PIPEDA in Canada and HIPAA in the USA, ensuring data privacy and security.
How much does prescription management software development cost?
The cost depends on features, integrations, compliance requirements, and customization level, ranging from basic solutions to complex enterprise systems.
Can DITS build prescription management software for Canadian and US healthcare businesses?
Yes, DITS develops tailored solutions that meet the specific regulatory and operational needs of healthcare businesses in both regions.
What features are essential for modern prescription management systems?
Key features include e-prescription capabilities, patient record management, drug interaction alerts, system integrations, and secure data handling.

Nidhi Thakur
With more than 19 years of experience - I represent a team of professionals that specializes in the healthcare and business and workflow automation domains. The team consists of experienced full-stack developers supported by senior system analysts who have developed multiple bespoke applications for Healthcare, Business Automation, Retail, IOT, Ed-tech domains for startups and Enterprise Level clients.
Recent Posts

Discover the benefits of AI in EHR system for Canadian clinics, including smarter documentation, patient engagement, risk detection, and operational efficiency.

Discover how outsourced software product development services help businesses reduce development costs, access specialized talent, accelerate delivery, and improve scalability.

Build scalable mobile apps for startups & enterprises with expert development, seamless UX, and faster launch.